|
Surg Endosc 18:646–649ĭorfman RE, Alpern MB, Gross BH, et al. Koler AJ, Lilly MC, Arregui ME (2004) Suprapancreatic and periportal lymph nodes are normally larger than 1 cm by laparoscopic ultrasound evaluation. (1997) Enlargement of perihepatic lymph nodes in relation to liver histology and viremia in patients with chronic hepatitis C. Br J Radiol 80:841–848ĭietrich CF, Lee JH, Herrmann G, et al. Morón FE, Szklaruk J (2007) Learning the nodal stations in the abdomen. (2007) Enlarged abdominal lymph nodes in end-stage cirrhosis: CT-histopathologic correlation in 507 patients. Clin Gastroenterol Hepatol 4:1373–1377ĭodd GD 3rd, Baron RL, Oliver JH 3rd, et al. (2006) Periportal lymphadenopathy in patients without identifiable pancreatobiliary or hepatic malignancy. Krishna NB, Gardner L, Collins BT, et al. Goldberg HI (1994) What is the significance of periportal adenopathy in a patient with hepatic cirrhosis? AJR Am J Roentgenol 163:742 (1990) Prevalence and significance of abdominal lymphadenopathy in patients with chronic liver disease: an ultrasound study. Our study suggests that no follow-up of PCLA is required in these settings.Ĭassani F, Zoli M, Baffoni L, et al. 
Conclusionsĭevelopment of malignancy is rare in patients with PCLA, either incidental or secondary to cirrhosis or chronic viral hepatitis. Of these, 42 (87.5%) had ≥6 months follow-up (median 28 months), and only 1 patient developed cholangiocarcinoma (positive predictive value 2.4%). Cirrhosis or chronic viral hepatitis was present in 48 (10.0%) patients. No patient with incidental PCLA developed malignancy in organs drained by these nodes. Of these, 112 (76.7%) had ≥6 months of follow-up (median 26 months). 
PCLA was incidental in 146 (30.5%) patients. In 285 (59.5%) patients, PCLA was explained by local pathology or systemic lymphadenopathy. ResultsĤ79 patients met inclusion criteria. Clinical or imaging follow-up ≥6 months was performed to detect if malignancy developed in organs drained by portacaval nodes in patients with incidental PCLA, cirrhosis, or chronic viral hepatitis. Records were reviewed for presence of malignancy, liver metastases, chronic viral hepatitis, and cirrhosis. We searched CT reports from 2005 to 2007 for the phrases “periportal node” and “portacaval node.” MDCTs of patients with portacaval nodes ≥10 mm in maximal short-axis size on contrast-enhanced MDCTs, were included. We aimed to detect the incidence of malignancy in organs drained by portacaval nodes in patients with PCLA associated with cirrhosis or chronic viral hepatitis, or incidentally detected PCLA. Besides neoplastic, inflammatory, and infectious processes, many other disease processes may occasionally result in mesenteric lymphadenopathy.Portacaval lymphadenopathy (PCLA) is common in cirrhosis and chronic viral hepatitis and is frequently an incidental finding on abdominal CT scans. 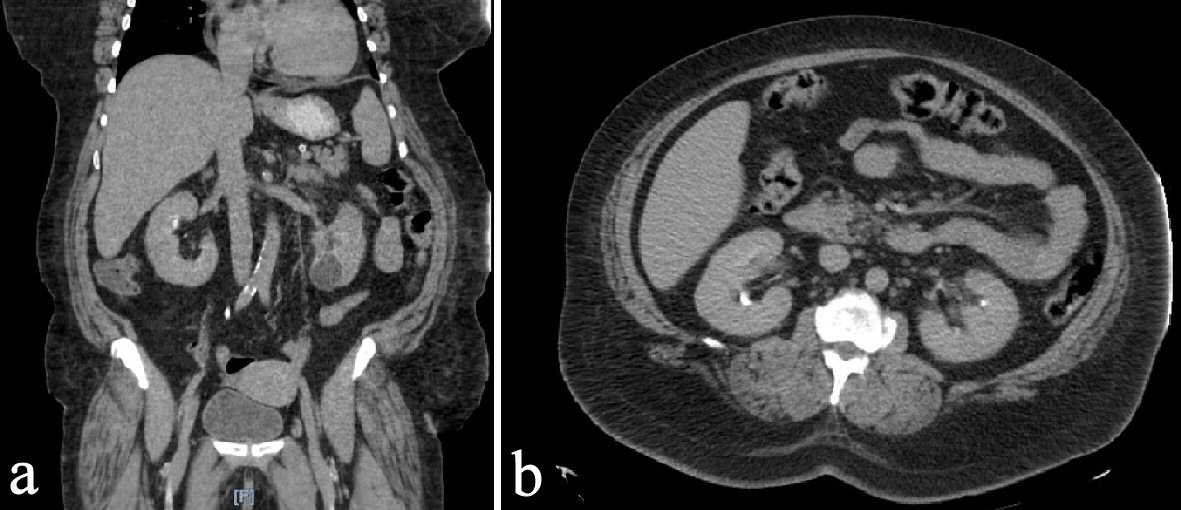
The distribution of the lymph nodes may indicate the exact nature of the underlying disease process, and the correct treatment may then be instituted. In addition, mesenteric lymphadenopathy may be the only indicator of an underlying inflammatory or infectious process causing abdominal pain. It is important to recognize mesenteric lymphadenopathy in patients with a history of a primary carcinoma because the lymphadenopathy affects the staging of the disease, which in turn will affect further management. Many of these causes may also result in lymphadenopathy elsewhere in the body. The most common causes of mesenteric lymphadenopathy are neoplastic, inflammatory, and infectious processes. Although the detected lymph nodes may be normal, there is a large number of disease processes that may lead to mesenteric lymphadenopathy. Because of the increasing volume of cross-sectional imaging examinations being performed, lymph nodes in the mesentery are being detected with increasing frequency. For the first time, normal mesenteric nodes may be reliably identified noninvasively. With the advent of multidetector computed tomography, routine evaluation of mesenteric lymph nodes is now possible.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
